Effective revenue cycle management in healthcare is crucial for practices taking their financial health and longevity seriously. However, the use of low-code apps for revenue cycle management (RCM) and other analytics tools has historically been leveraged mostly by large healthcare systems, hospitals, and management service organizations (MSOs) that have the budget to invest in the development of said tools.
Additionally, given the acquisition activity with providers, the challenges for mid-market practices navigating patient acquisition and payer relations only increase. Denials and accounts receivable issues further strain cash flow and operations, making the need for an RCM increasingly vital.
So how can mid-market dental and medical practices enhance their revenue cycle management in a cost-friendly way that also measures up to enterprise-level solutions?
Read on to learn how.
The Problem of Denied Claims
Denied claims not only disrupt cash flow but also create substantial challenges to mid-market practices trying to maintain sustainable business operations in an increasingly competitive industry.
In essence, a denied claim represents a missed opportunity for revenue generation. For small to mid-sized practices, the impact is particularly pronounced, as they often lack the resources and infrastructure to effectively manage and mitigate denials. This is becoming an ever-increasing issue, with initial denial rates increasing from 10% in 2020 to nearly 12% in 2022.
Common reasons for claim denials in the healthcare industry include incomplete or inaccurate information, non-covered services, and coding errors.
The administrative burden of managing denials is further compounded by the disjointed nature of traditional revenue cycle management methods. Manual processes, often reliant on spreadsheets, lead to version control issues and inefficiencies, while legacy electronic health record (EHR) systems fail to provide seamless integration with revenue cycle management functions.
The Microsoft Power Platform, coupled with the latest AI advancements, offers a solution for managing denied claims for mid-market businesses, significantly enhancing the accessibility and ease of implementing RCM solutions. But first, let’s get a better picture of the current state of revenue cycle management for healthcare.
Current Approaches to Revenue Cycle Management
Traditionally, providers have relied on manual processes or legacy systems to manage revenue cycles, leading to inefficiencies and missed opportunities for optimization.
Manual methods, such as spreadsheet-based tracking, lack real-time visibility and are prone to data entry and process errors. Legacy EHR and patient administration systems, while central to patient care, often lack the sophistication required for comprehensive revenue cycle management, leading to siloed data and fragmented workflows.
Additionally given the high turnover rates of billing and office staff, relying on manual and opaque processes, leaves practices constantly training and retraining staff just to manage the existing process, leaving little time to make process improvements.
For truly efficient RCM, all these systems need to talk to each other and allow their users to visualize real-time data. By leveraging the Microsoft Power Platform for process management, automation, and data analytics, we can unlock the full potential of revenue cycle management. This allows healthcare organizations to streamline processes, identify revenue leakage, and improve overall financial performance.
The Solution by SolisRx: Low-Code Apps, Analytics, and AI Delivered in Weeks
Microsoft Power Platform has revolutionized the landscape for mid-market healthcare businesses, offering a gateway to harness analytics and unlock the potential of their data. At SolisRx, we’re leveraging this transformative technology to empower organizations and improve their RCM, allowing them to extract actionable insights, optimize processes, and drive informed decision-making.

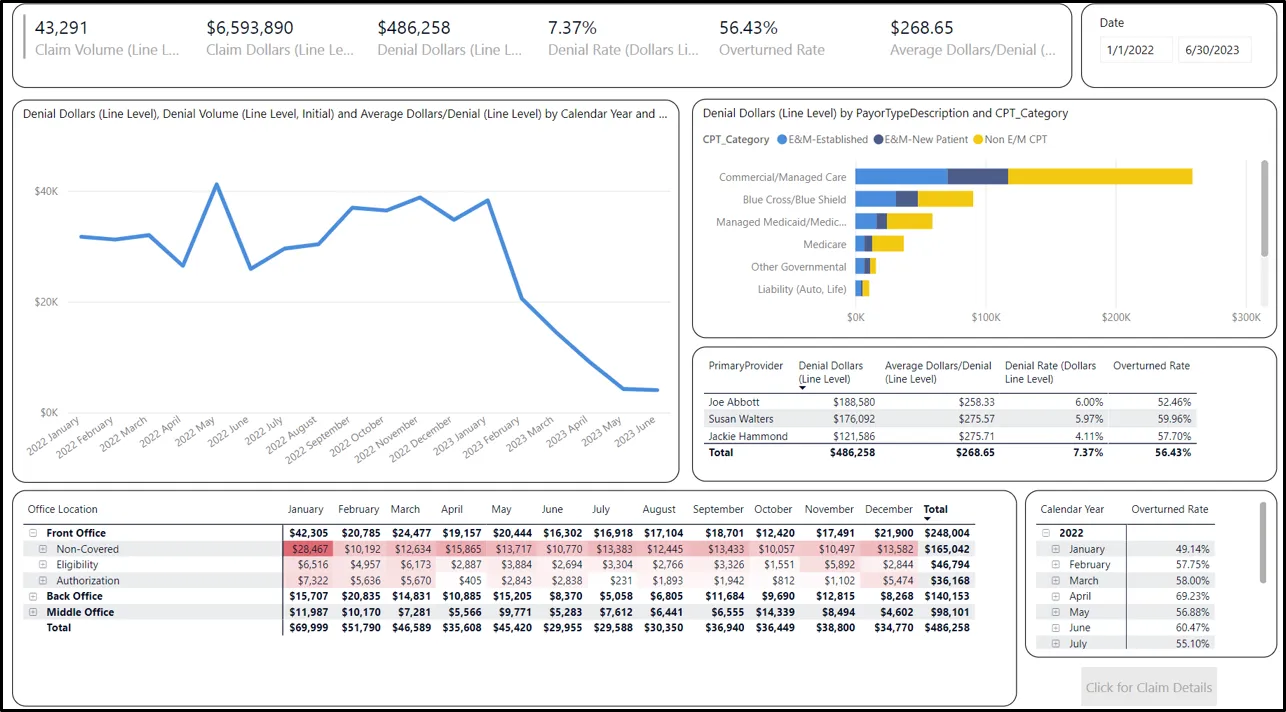
This solution used Power Automate to automatically acquire, ingest, and analyze all denied claims out of the provider's EHR/EDI feeds and visualize them in easy to use Power BI reports. This dashboard allows users to see denied claim volume and dollars cut by Time, Provider, Payer, CPT Code, Claim Adjustment Reason Code (CARC), Remittance Advice Remark Code (RACR), etc.
Specific insights and value sources that can be unlocked are:
- See a report of denied claims by Time, Provider, Payer, CPT Code, CARC, RACR, etc. to understand where your denials are coming from
- Place your existing denied claims into bespoke workflows for your Revenue Cycle teams to manage. Track each claim by status and team member to know exactly where each claims sits and how likely it is to be overturned and when the overturn might occur
- Use the insights of knowing the largest source of your denials in point #1, to conduct focused "Root Cause Analysis" exercises, which includes shadowing your existing processes and staff members to understand what part of your operations are causing the denials to occur. Once you have this understanding, you can implement process changes to prevent the denials from occurring in the first place.
An Overview of the Power Platform
Microsoft's Power Platform encompasses a suite of powerful tools, including Power BI, Power Apps, and Power Automate, designed to empower users with unparalleled capabilities in data analysis, application development, and workflow automation. By leveraging these tools, we can help SMBs accelerate their digital transformation journey while enjoying several key advantages:
- Affordability: Power Platform can reduce development costs by 74%, enabling SMBs in healthcare to harness advanced analytics without breaking the bank.
- Increased Data Security: Built on Microsoft's robust security infrastructure, the Power Platform ensures data integrity and HIPAA compliance. This includes role-based access control and data logging.
- Faster Development: With intuitive interfaces and low-code development capabilities, the Power Platform accelerates the application development process, allowing organizations to bring solutions to market in weeks instead of months or years.
- Instantiate Best Practices: Move beyond outdated and error-prone spreadsheet-based processes. Instead, build software that can manage your complex processes with the right mix of automated vs manual workflows that is easy to onboard and train new staff regardless of their technical background.
- Seamless Integration: Seamlessly integrated with Microsoft 365 products, the Power Platform enables businesses to leverage their existing investments and maximize efficiency across their ecosystem. Such as automatically sending email follow-ups regarding denied claims to internal team members or payers as shown below.

The Benefits of Partnering with SolisRx
SolisRX has 10+ years of expertise in the healthcare industry, offering custom solutions to address the challenges mid-market practices face, particularly regarding RCM. By partnering with us for your low-code apps for revenue cycle management, organizations can experience multiple, including:
- Deep Healthcare Expertise: With a founding team boasting extensive experience in the healthcare technology sector, SolisRx understands the intricacies of revenue cycle management, denied claims, and value-based care, uniquely positioning us to deliver impactful solutions
- Affordable Rates and Innovative Delivery Model: SolisRx adopts an innovative delivery model that combines onshore and nearshore resourcing, allowing organizations to access top-tier talent at competitive rates. This approach ensures cost-effectiveness without compromising on quality or scalability.
- Low-Code Solutions with HIPAA Compliance: SolisRX offers low-code solutions that prioritize security and compliance, ensuring adherence to HIPAA regulations and safeguarding sensitive patient data.
“Unlike an Excel spreadsheet under your desk or access database, all interactions are happening as an authenticated user, so you can apply controls and access policies” Ryan Cunningham, VP of Power Apps

Get Low-Code Apps for Revenue Cycle Management with SolisRx
By now it’s clear that effective revenue cycle management is imperative for the financial well-being of healthcare organizations, particularly small to medium-sized providers. By addressing the problem of denied claims and embracing our innovative solutions, practices can optimize revenue cycles, improve cash flow, and ultimately enhance patient care delivery.
Ready to transform your revenue cycle management operations? Explore the potential of custom dashboards built on Microsoft's Power Platform with SolisRx. Book a FREE 30-min consultation to learn more about our affordable, HIPAA-compliant solutions and take the first step towards unlocking the full potential of your healthcare organization's revenue cycle management.






